Shot in the Face at 24 — Then a 25-Hour Miracle Gave Him a New Face and a Second Life!
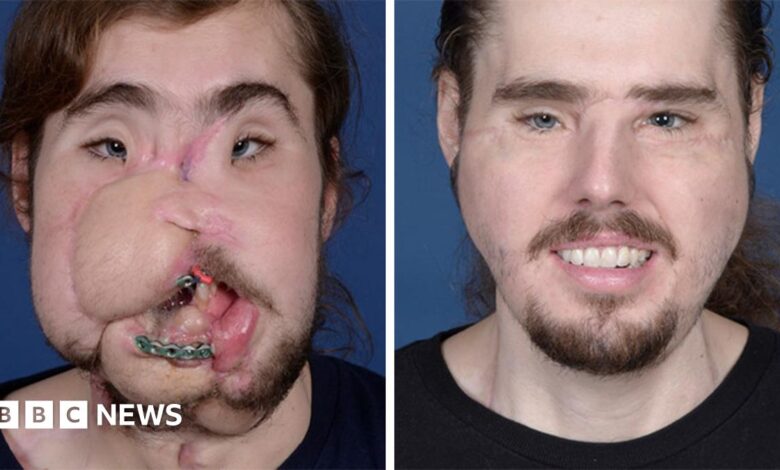
In January 2018, 26-year-old Cameron Underwood from Yuba City, California, made medical history as one of the youngest and fastest-recovering recipients of a full face transplant, marking a profound turning point after a devastating self-inflicted gunshot wound to the face in June 2016.The injury was catastrophic: the bullet obliterated his nose, most of his lower jaw, nearly all of his teeth (leaving just one), the roof and floor of his mouth, parts of his tongue, and lower eyelids, while severely impairing his vision, speech, and ability to eat anything beyond liquids through a feeding tube. For nearly two years, Cameron lived in isolation, facing constant stares, profound difficulty communicating, inability to eat solid food, and deep emotional scars from the suicide attempt that had left him disfigured and struggling to envision a future.His path to recovery began when his mother, Beverly Bailey-Potter, read an article about pioneering reconstructive surgeon Dr. Eduardo D. Rodriguez, the Helen L. Kimmel Professor of Reconstructive Plastic Surgery and chair of the Hansjörg Wyss Department of Plastic Surgery at NYU Langone Health in New York City. Dr. Rodriguez, who had previously performed the hospital’s first face transplant on firefighter Patrick Hardison, agreed to take on Cameron’s case.
Cameron traveled across the country to enroll in NYU Langone’s renowned Face Transplant Program, undergoing extensive evaluations, psychological support, and preparation.On January 5, 2018, a multidisciplinary team of more than 100 specialists—including surgeons, nurses, anesthesiologists, immunologists, and rehabilitation experts—performed what was described as the most technologically advanced face transplant to date in the United States. The groundbreaking 25-hour marathon surgery involved meticulously procuring and transplanting donor tissue from a deceased individual, reconstructing vast portions of Cameron’s face: the entire midface and lower face, both upper and lower jaws (including all 32 teeth and gums), the nose, tongue reconstruction, the roof and floor of the mouth, lower eyelids, and associated soft tissues and blood vessels.
The procedure incorporated innovative tools like a 3D-printed donor facial mask for precise planning and alignment, ensuring optimal functional and aesthetic outcomes.Post-surgery, Cameron faced an intense recovery period involving anti-rejection medications, physical therapy, speech therapy, orthodontic adjustments, nutritional counseling, and psychological support—much of it facilitated by organizations like myFace, which provided housing, travel, and rehab resources. Remarkably, his recovery progressed faster than expected: within months, he regained the ability to speak clearly, eat solid foods independently, smile naturally, and perform everyday activities.
Notably, Cameron experienced no acute rejection episodes in the first year and a half post-transplant—a rare feat shared only with NYU Langone’s prior patient—sparking scientific interest in the immune protocol used.In late November 2018, less than 11 months after surgery, Cameron publicly revealed his transformed face in interviews with outlets like CNN, BBC, TIME, and People Magazine. Visibly emotional, he described the transplant as “a second chance at life,” expressing gratitude to his donor (whom he later met with the donor’s family in a heartfelt reunion) and the medical team. He highlighted regained joys like smiling without hesitation, eating steak, golfing, restoring cars, and even skydiving—simple pleasures that had once seemed impossible. Cameron also emphasized the importance of sharing his story to raise awareness about mental health, suicide prevention, and the life-changing potential of face transplantation.Today, Cameron’s journey stands as an inspiring testament to medical innovation, resilience, and hope: from near-total facial loss and profound despair to restored function, confidence, and a renewed sense of normalcy. His case continues to advance the field of vascularized composite allotransplantation, offering renewed optimism for others facing similar catastrophic injuries.




